
Acting ahead of schedule, the FDA has granted an accelerated approval to ibrutinib as a treatment for patients with mantle cell lymphoma who have received at least one prior therapy.

Acting ahead of schedule, the FDA has granted an accelerated approval to ibrutinib as a treatment for patients with mantle cell lymphoma who have received at least one prior therapy.

The role of transplant in MCL is in clinical evolution. Up-front high-dose therapy and autologous stem cell transplant remains an attractive option for those with chemosensitive disease regardless of the induction regimen chosen, whereas this approach in the relapsed or refractory setting has not yielded long-term disease-free intervals.

The Cancer Genome Atlas provides us with our first thorough insight into the genetic heterogeneity of squamous cell carcinoma of the lung; whether these findings will translate into personalized squamous cell lung cancer therapy is yet to be determined.

The standard of care for metastatic renal cell carcinoma (RCC) prevailed in a randomized comparison of everolimus (Afinitor) and sunitinib (Sutent) as first-line therapy

Researchers have had little success in developing an HIV cure, but recent studies involving gene therapy, immune-based therapy, reactivation of the immune system, and "very early" treatment have produced promising results.

The ratio of two protein levels may predict clinical benefit of EGFR inhibitors. Low levels of a protein called Mig6 (mitogen-inducible gene 6) and high levels of EGFR corresponded to a higher clinical response rate and progression-free survival in a small prospective cohort of lung cancer patients treated with the anti-EGFR therapy gefitinib.
A phase III trial exploring necitumumab plus chemotherapy as a first-line therapy for patients with metastatic squamous non-small cell lung cancer has demonstrated an improvement in overall survival when compared to chemotherapy alone.

The FDA approved afatinib (Gilotrif) as a first-line therapy for patients with metastatic non-small-cell lung cancer whose tumors harbor certain mutations in the epidermal growth factor receptor gene.

A two-step immunotherapy approach consisting of adoptive T-cell therapy and a dendritic cell vaccine has shown activity in a phase I advanced ovarian cancer clinical trial.
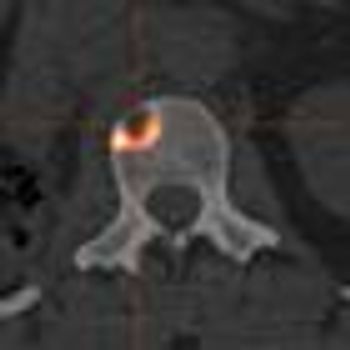
Bone metastases result in poorer outcomes for those patients with advanced renal cell carcinoma (RCC), who were treated with a molecularly targeted therapy. The results were presented in two separate analyses at the annual ASCO meeting.

Patients with chronic lymphocytic leukemia and mantle cell lymphoma showed high response rates to therapy with the novel targeted therapy ibrutinib, further solidifying the safety and efficacy of a drug that has proven very promising in early clinical trials.
Researchers observed durable responses in patients with renal cell carcinoma treated with the PD-L1 antibody MPDL3280A. The study, which was presented at the 2013 ASCO Annual Meeting, was one of the few immune therapy trials that allowed patients with non-clear cell histologies and some clinical activity was observed in these patients.

Salvage therapy combining the novel heat shock protein 90 inhibitor ganetespib with docetaxel significantly improved overall survival in some patients with non–small cell lung cancer.

A simple serum protein test can help guide treatment decisions between chemotherapy and erlotinib as second-line therapy for patients with non-small-cell lung cancer, according to results of a phase III study presented at ASCO.

Ian MacDonald, MSc, MD, talked about the future of gene therapy trials in choroideremia, a single-gene disorder that primarily affects the eye.

Within the relatively short time that ipilimumab and vemurafenib have been commercially available, phase II data for the investigational agents nivolumab and MK-3475, for the combination of dabrafenib and trametinib, and for adoptive cell therapy strongly suggest even further improvements in treatment outcomes.

A new compound shows potential as a novel targeted therapy for retinoblastoma. While studies are still in the preliminary stages, the compound known as sd-rxRNA was able to penetrate all cell layers of the retina and was taken up by tumor cells within 24 hours of intravitreal administration, said Michael Byrne, PhD.

Phase III study of RPE65 for Leber’s congenital amaurosis under way, among other research

Phase III study of RPE65 for Leber’s congenital amaurosis under way, among other research
A dose-adjusted regimen of etoposide, doxorubicin, and cyclophosphamide with vincristine, prednisone, and rituximab (DA-EPOCH-R) obviated the need for radiotherapy in patients with primary mediastinal B-cell lymphoma in a single-group, phase II, prospective study.

The Wnt signaling pathway was demonstrated as a promising target in cancer stem cell therapy through a series of talks highlighting the promise and efficacy of a new generation of inhibitors that are making their way into the clinic.

After receiving breakthrough therapy designation from the FDA for the treatment of two B-cell malignancies earlier this year, ibrutinib has received an additional breakthrough designation.

The compound LDK378, a highly selective inhibitor of ALK, has been granted "Breakthrough Therapy Designation" by the FDA for the treatment of patients with ALK-positive metastatic non-small cell lung cancer.

Although the presence of an EGFR mutation is a predictive marker for response to EGFR tyrosine kinase inhibitor therapy in patients with non-small cell lung cancer, the mutation is not a prognostic factor.

A trial comparing axitinib to sorafenib as first-line therapy for metastatic renal cell carcinoma showed a statistically significant improvement in progression-free survival for the drug; however, the difference failed to meet the phase III trial’s prespecified significance level of 0.025.

Axitinib did not demonstrate superiority over sorafenib as first-line therapy for patients with metastatic renal cell carcinoma, on the endpoint of progression-free survival.

Tivozanib did not show a significant difference in overall survival when compared with sorafenib in patients with renal cell carcinoma who received up to one prior line of therapy excluding targeted agents.

Combination targeted therapy did not significantly extend progression-free survival compared with single-agent bevacizumab in patients with advanced renal cell carcinoma.

The investigational agent ibrutinib was granted "Breakthrough Therapy Designations" by the FDA as a singular therapy for a pair of B-cell malignancies: relapsed or refractory mantle cell lymphoma and Waldenström's macroglobulinemia.

As therapy based on cell-signaling pathways has become a priority in cancer research, so has the concept of designing clinical trials that can better target patient populations more likely to benefit from a particular regimen.